Leg casts and blood clots, reducing the risks
Information about how to reduce the risk of deep vein thrombosis (DVT) and pulmonary embolism (PE) during and after having your leg immobilised in a plaster cast or other appliance such as a splint or boot.
What are blood clots (VTE)?
Your blood has a mechanism that normally forms a blood clot (plug) to stop the bleeding when you are injured (example: when you have a cut). Sometimes this mechanism can go wrong and forms a blood clot without an injury, which can block the vein and stop the blood flowing to the affected area.
This is called venous thromboembolism (VTE), which can happen:
In a vein of the leg causing a deep vein thrombosis (DVT)
If the DVT becomes loose, it can travel to the lungs causing a pulmonary embolism (PE). This condition can be fatal.
- DVT can lead to post-thrombotic syndrome on the leg (permanent pain, difficulty walking, leg wounds that don’t heal).
- PE when not fatal, can lead to chronic pulmonary hypertension (weak heart, chest pains, shortness of breath).
Why am I at risk?
People with a leg immobilised in any form of plaster cast, boot or brace following a fracture or injury are more likely to develop VTE.
Being active, particularly walking, helps pump the blood around the body. When the leg is immobilised, it stops you being able to move as freely as you were able to before your injury. The increased risk of developing VTE happens as a result of a slower blood flow to the legs.
The risk of VTE varies between patients as other risk factors come into play. That is why it is crucial that all patients are assessed for their risk of VTE to establish their personal risk level.
VTE Risk Factors
Related to You
- Being over 35 years of age
- Being overweight (BMI ≥25)
- Having had cancer in the last 5 years
- Having other health conditions, for example: diabetes, asthma, high cholesterol, heart disease, arthritis, thrombophilia and other clotting disorders, varicose veins, high blood pressure …
- Dehydration
- Pregnancy or 6 weeks after birth
- Being Male
- You or your family member having a VTE in the past
- Taking the contraceptive pill or HRT
- Recent: operation, hospital admission, long journey (plane, train, car, bus)
Related to your injury
- A severe injury (eg. dislocation, fracture, complete tendon rupture)
- A long, short or half cast or splint
- If you are not allowed to put weight on the leg, using crutches
- A significant reduction in your mobility, spending long periods housebound, in bed or chair
It is a good thing to know your risk so you can do something about it.
Having risk factors does not mean you will have VTE.
Not having risk factors also doesn’t mean you will not get VTE. There are lots of things you can do to reduce the risk of VTE.
How to reduce the risk?
General recommendations for all patients with leg casts:
Stay Active
Drink Plenty
VTE Prevention Exercises
VTE Prevention Exercises
These exercises increase the blood flow to the legs and to the lungs helping to prevent VTE. To be able to do them you may need to take painkillers regularly, as pain is a common reason for people not moving about increasing the risk of VTE.
Do 10 repetitions of each exercise every hour, while you are awake.
Exercises for the injured leg: You can do them with any type of cast
Whilst your leg is immobilised you will find it difficult to have a full range of movement.
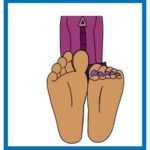
Wiggle your toes while lying in bed or whilst sitting up with your legs elevated.

Paddle your feet up down and circle them around and around. The circle motion should be clockwise and then anticlockwise.
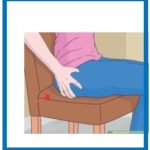
Buttocks squeezing Lying down or sitting, clench your buttock muscles together and hold for a count of 3 before relaxing.
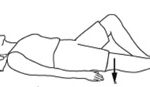
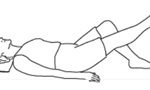
Static Quads and lifts
Lie down, with kneecap and toes facing the ceiling. Tighten the muscles in the front of the thigh and push the back of your knee into the bed holding for 3 seconds and then relax.
To do the lift, raise your leg from the bed with the knee held straight, hold it for 3 seconds and gently bring the leg down.
Exercises for the injured leg: only for below knee cast
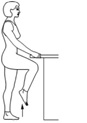
Knee bends and lifts Hold on to a table or counter for support. Slowly bend your knee by lifting your heel towards your buttocks. Hold for 3 seconds. For the lifts slowly raise your knee up to the level of your hip, hold for 3 seconds. Slowly lower your foot to the floor.
Exercises for the good leg:
All exercises for the injured leg can be done on the good leg, as well as:
Sit to standing: Sitting on a chair, holding on to a table or counter, stand up and sit back down slowly, keeping your back straight.
Paddle your feet up and down and circle them around and around. The circle motion should be clockwise and then anticlockwise.
Breathing Exercises:
Place your hands on the side of your rib cage. Take a slow deep breath and feel the ribs being pushed upwards and out to the side as you expand your lungs. Hold it for 3 seconds. Breathe out slowly with your lips closed together as if you are whistling.
How to reduce the risk?
To reduce your risk of VTE all you have to do is follow the general recommendations for all people with a leg immobilisation:
- Stay Active
- Drink Plenty
- VTE Prevention Exercises
The doctor or nurse will complete a VTE risk assessment to take into account all of your risk factors. Depending on the assessment, you may also require anticoagulant medication.
Anticoagulant medication
Anticoagulant medication modifies the blood clotting process to stop clots forming so easily. The injection normally prescribed is called ‘Dalteparin’ and is usually injected beneath the skin into a skin fold over your stomach. This will be done every day for as long as you have your leg immobilised (up to 8 weeks).
The nurse will teach you how to do this injection and provide you with instructions on Dalteparin injections plus a yellow sharps bin to store all the used syringes safely.
The good news is:
- The injection is ready to use, no fiddling about
- The needle is one of the smallest (1.2 cm long)
- The liquid to inject is also very little (0.2 ml)
- The injection procedure is easy
- It feels like minor stinging
- It only takes about 20 seconds
- Alternative arrangements are available if you can’t do it
Find out more about Dalteparin injections
Anticoagulants – Contraindications
You should not be offered anticoagulant medication if you …
- Are bleeding
- Have low a platelet count (less than 50)
- Have poor kidney function
- Have had a recent spinal, brain or eye operation
- If you are already taking anticoagulant medication (eg: for your heart)
Best practice for maximum benefit:
- Make sure you take it as prescribed
- Take it every day at the same time/times
- Do not miss any doses
- Keep an eye out for complications (see next section (‘complications’)
- Any problems with your anticoagulant medication, contact your GP immediately
Complications
Be aware of the following uncommon complications of taking anticoagulant medication:
- Allergy (example: rash, severe reaction: anaphylaxis) Extreme tiredness or pallor
- Extreme bruising or bleeding
(for example: nosebleeds, blood in the urine or stools, bleeding from surgical wounds, heavy periods, internal bleeding, bruising on your stomach at the injection site, easy bruising)
If this happens, call your GP immediately. For severe reactions: bleeding that doesn’t stop or anaphylaxis call 999 immediately.
How do you know if you have VTE?
Unfortunately, even if you are at low risk and follow all of the advice to prevent VTE, you may still get it.
Signs and symptoms
- Swelling of the leg or calf
- Pain that may worsen when standing or walking
- Warmth and redness of the leg
If you suspect you have a DVT call your GP as soon as possible!
- Unexplained sudden breathlessness
- Sudden sharp chest
- Coughing up blood
This is an emergency. If you suspect you have a PE call 999 immediately!
Useful information:
Buckinghamshire Hospitals Trust Patient Medicines Helpline: 01296 31 6197
National Institute for Health and Care Excellence: Venous thromboembolism in over 16s: reducing the risk of hospital-acquired deep vein thrombosis or pulmonary embolism
DVT (deep vein thrombosis) – NHS (www.nhs.uk)
Download the App Preventing VTE (found in Google Play)
