Colposcopy appointment
What is Colposcopy?
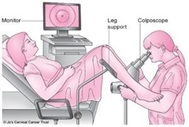
A colposcopy is a detailed examination of the cervix (neck of the womb) which normally occurs after a patient has had an abnormal smear result. A Colposcope is a special magnifying instrument which allows the doctor or specialist nurse to get a clear view of the cervix. Sometimes the vagina and the vulva (the folds of skin outside the vagina) are examined at the same time. A colposcopy is carried out by a doctor or a specially trained nurse as an outpatient procedure, accompanied by a Staff Nurse and Health Care Assistant who are present to support both you and the doctor. The colposcopy examination should not cause any pain, but some may find it uncomfortable.
What causes an abnormal smear?
Abnormal smears are common: 1 in 10 smears will show an abnormality. Mild or borderline cell changes can often return to normal without treatment, and very few women with an abnormal smear have cancer. Abnormal smears are reported if pre-cancerous (dyskaryotic) cells are found. Pre-cancerous changes are usually associated with Human Papilloma Virus (HPV or wart virus), which is very common and many women will have been exposed to it at some point in their life.
Anybody who has ever been sexually active is at risk of acquiring a type of HPV that can change cells in the cervix. It is transmitted primarily by skin to skin contact, including genital to genital contact, anal intercourse and oral sex. Time between exposure to HPV and the development of cervical abnormalities is variable and HPV can remain dormant in some people for long periods of time.
Smoking cigarettes
There is evidence to suggest that smoking cigarettes increases the risk of cervical abnormalities developing. Smoking alters the cell’s ability to protect themselves and to fight off infection.
The Colposcopy examination
Please contact the Colposcopy Team if:
- Your appointment needs to be rescheduled
- You are pregnant or think you could be
- You are going on holiday within the next few weeks
- You require mobility assistance
- You have had previous colposcopy problems
- You are being treated for any vaginal infections
- You have health problems i.e. taking blood thinning medication, allergies or autoimmune medication.
Prior to your appointment please:
- Eat and drink as normal
- Have someone bring you to, and take you home from, the hospital if this will make you feel more comfortable
- Wear a loose skirt to your appointment if you find it easier but please do not apply moisturiser to your legs
- Avoid sexual intercourse 24 hours prior to your appointment
- Refrain from sexual intercourse 5 days prior to your appointment if you have a coil or use additional alternative methods of contraception during this time
- Avoid using vaginal creams, intimate hygiene products or pessaries
- Have your period cycle information i.e. first day and last day of your period
- Let us know if you are having any colposcopy treatment or care in any other setting
- Let us know if you have any medical alerts
What happens during colposcopy?
You will meet a doctor or nurse called a Colposcopist and your examination will take place on a special chair/couch. They will use a type of microscope with a light at the end, a Colposcope, to take a closer look at your cervix. A speculum will also need to be inserted to allow visualisation of the cervix. They may offer you tests to help diagnose cell changes and decide whether you need treatment, including:
- using different liquids to stain your cervix and show any cell changes
- a biopsy, where a small piece of cervical tissue is removed – it is then sent to the lab for testing
If you need treatment it may be offered during your first colposcopy appointment, or you may be invited back to have treatment at another appointment. The option you are offered may be due to the colposcopy tests and the opinion of the Colposcopist, but both are as good as each other. If you are offered treatment during your first appointment, it is okay to ask for time to think about it, either at the appointment or at home. Your Colposcopist should invite you to have a seat away from the examination bed to talk you through the treatment and answer any questions. This is called ‘see and treat’.
You can read more about the colposcopy at www.jostrust.org.uk/colposcopy
LLETZ (large loop excision of the transformation zone)
LLETZ is the most common treatment for cervical cell changes. A thin wire loop with an electrical current is used to remove the affected area of the cervix.
Your LLETZ Appointment
Your appointment will take place in a Colposcopy Clinic at a hospital. You usually have a LLETZ as an outpatient. This means you have the treatment in a hospital examination room, and you can go home afterwards.
You usually have a local anaesthetic for a LLETZ, but you can choose to have it done under general anaesthetic, where you will be asleep.
The hospital wants to keep you and their staff protected from COVID-19 (Coronavirus), so they will be following government guidance on social distancing and using appropriate personal protective equipment (PPE), including masks, gloves and aprons. You will also need to wear a face covering whilst in the hospital.
If you take blood thinning medication, or have a condition that affects your blood, it is important to tell your Colposcopist before your appointment. You may have a higher risk of bleeding after the treatment and may be advised to suspend your blood thinning medication for 1-2 days prior to your appointment.
After your treatment- what can you expect?
Bleeding – bleeding is expected after a LLETZ and can last from 2 days up to 4 weeks. You may have bleeding because of the soft scab that forms on the cervix where the cells were removed, which may bleed whilst it heals.
The bleeding is usually like a period but may be slightly heavier than your normal period. About 10 days after treatment the bleeding may get heavier. This is common and is a sign that the scab is healing. Your first period after treatment may be slightly heavier or ‘out- of-sync’ with your regular cycle.
If the bleeding is soaking through a period pad every hour, call the contact number given by your Colposcopy Team 01296 838888 or call 111 out of hours. This is sometimes called delayed haemorrhaging and the hospital Team or 111 will be able to advise you and make sure you get the right care.
Pain – Some pain is expected from 2 days to up to 4 weeks after treatment. The pain varies from person to person but should not be too severe. It is often described as a cramping pain, like a period. You can talk to your doctor about over-the-counter medication which should help.
Changes to Vaginal Discharge – Changes to vaginal discharge can last for about 4 weeks. Straight after treatment you may have a watery, brown vaginal discharge.
About 10 days after treatment, you may notice a coffee granule-like vaginal discharge. This is normal and a sign that the soft scab on your cervix is healing.
Between about 1 – 14 people in 100 (0.8% to 14%) get an infection after a LLETZ. Talk to your GP if your vaginal discharge smells bad or is a yellow or green colour. If there is a chance you have an infection, you will be offered antibiotics.
What can I do or not do after a LLETZ?
You may have some physical effects after a LLETZ (see below where you can obtain further information). These usually last up to 4 weeks but until these have stopped, it is best to avoid:
- tampons or menstrual cups – you can use a period pad instead
- penetrative vaginal sex – including fingers and other objects
- heavy exercise that causes you to sweat, such as running or a gym workout
- swimming
- long baths – you can continue to shower as normal
Results
Tests/biopsies/treatment – when the histology (microscopic examination of biopsies) is reviewed (about 4-6 weeks) the Colposcopist will write to you and your GP with the result and a plan of management.
Helpful Information
We advise you to allow adequate time to get to the Clinic and for parking which is limited.
If you have any additional needs, please contact us on 01296 838888 or bht.colposcopy@nhs.net
For further information please view:
