Pelvic Floor Repair (Anterior and Posterior) without the use of mesh
The information provided here should be used as a guide for women who have been advised to have a pelvic floor repair. It outlines common reasons for the operation, benefits, risks, recovering from the operation and what to expect when you go home. You should ask your Gynaecologist about any concerns that you may have.
This information describes anterior as well as posterior vaginal repairs using your own tissues and without the use of mesh (native tissue repair).
What is prolapse?
The pelvic floor muscles form a hammock across the opening of the pelvis. These muscles, together with their surrounding tissue are responsible for keeping the pelvic organs (bladder, uterus, and rectum) in place. Prolapse occurs when the pelvic floor muscles, their attachments or the vaginal tissue become weak. This usually occurs because of damage at the time of childbirth but is most noticeable after the menopause when the quality of supporting tissue deteriorates. It is also related to chronic strain caused by heavy lifting, repeated coughing and constipation.
What is anterior vaginal wall prolapse?
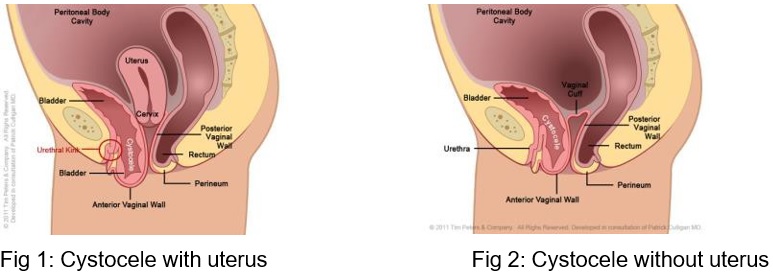
An anterior vaginal wall prolapse (also called a cystocele) is a prolapse of the front wall of the vagina with the bladder bulging into the vagina (Figures 1 and 2). This sometimes can be large and push out of the vagina especially on straining e.g. exercise or passing a motion.
A large cystocele may cause or be associated with urinary symptoms such as urinary leakage, urinary urgency (strong and sudden desire to pass urine), having to go frequently, difficulty passing urine or a sensation of incomplete emptying.
Some women have to push the bulge back into the vagina or lean forward in order to completely empty the bladder. Incomplete bladder emptying may make you prone to bladder infections (Urinary Tract Infection). Some women find that the bulge causes a dragging or aching sensation, or is uncomfortable when having sexual intercourse.
What is a posterior vaginal wall prolapse?
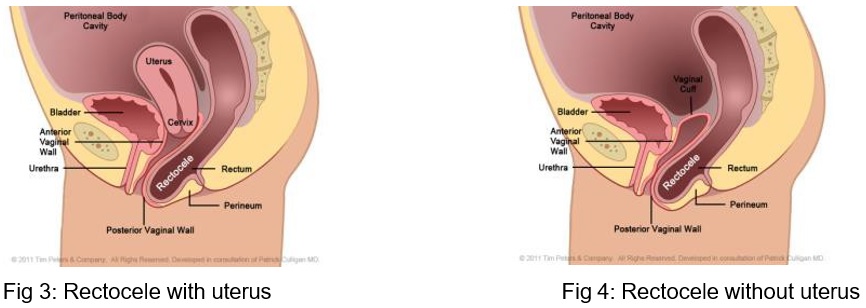
A posterior vaginal wall prolapse (also called a rectocele or a rectoenterocele) is a prolapse of the back wall of the vagina. The rectum (bowel) bulges through the vagina (Figures 3 and 4).
The perineum is the area between the vagina and the back passage. It provides some support for the vagina and may be damaged during childbirth. With straining, for example on passing a motion, the weakness described above allows the rectum (back passage) to bulge into the vagina and sometimes bulge out of the vagina (rectocele). A large rectocele may make it very hard to have a bowel movement especially if you have constipation. Some women have to push the bulge back into the vagina with their fingers, support the perineum or insert a finger in the back passage in order to complete a bowel movement. Some women find that the bulge causes a dragging or aching sensation.
What is an anterior repair?
An anterior vaginal repair (colporrhaphy) is an operation performed within the vagina to treat an anterior (front) vaginal wall prolapse also called a cystocele.
What is a posterior vaginal repair?
A posterior vaginal repair (colporrhaphy) is an operation performed within the vagina to treat a posterior (back) vaginal wall prolapse also called a rectocele. Posterior repair is often combined with a repair of the area between the vagina and the back passage, the perineum (perineorrhaphy).
How is the anterior or posterior vaginal wall repair done?
The operation is usually done under general anaesthetic. A general anaesthetic will mean you will be asleep during the entire procedure. A spinal anaesthetic can also be used which involves an injection in your back to numb you from the waist downwards.
The operation is all done vaginally and involves repairing the supportive tissues using dissolvable stitches. These stitches usually take 4-6 weeks to dissolve although some surgeons use sutures that take about 3-6 months to dissolve completely. This should not affect your recovery time. If the perineum is repaired, you might notice a few stitches on the outside but these will dissolve and fall away fairly quickly.
A catheter and a vaginal pack (gauze tampon) may be inserted in the vagina after the operation but this is not essential and depends on the surgeon’s preference and method of operating. These are usually removed the following day.
Other operations which may be performed at the same time
- Surgery for other types of prolapse; for example, a vaginal hysterectomy or a sacrospinous fixation or sacrohysteropexy to treat a prolapse of the uterus (womb) or the top of the vagina.
- Surgery to treat urinary incontinence.
You should also refer to an information leaflet about any planned additional procedure.
Benefits
The primary aim of the operation is to reduce the bulge within the vagina. There are benefits associated with this. You are likely to feel more comfortable. Intercourse may be more satisfactory. Your bladder and/ or bowels may empty more effectively and urinary frequency and urgency may be reduced.
Altered sensation during intercourse
Sometimes the sensation during intercourse may be less and occasionally orgasm may be less intense. On the other hand repair of your prolapse may improve it.
Risks
General Risks of Surgery
Anaesthetic risk
This is very small unless you have specific medical conditions, such as a problem with your heart, or breathing. Smoking and being overweight also increase any risks. A posterior repair can be performed with you asleep (a general anaesthetic) or awake but numb from the waist down (a spinal anaesthetic). This will be discussed with you.
What can you do?
Make the anaesthetist aware of medical conditions such as problems with your heart or breathing. Bring a list of your medications. Try to stop smoking before your operation. Lose weight if you are overweight and increase your activity.
Bleeding
There is a risk of bleeding with any operation. It is rare that we have to transfuse patients after their operation.
What can you do?
Please let your doctor know if you are taking a blood-thinning tablet such as warfarin, aspirin, Clopidogrel or rivaroxaban as you may be asked to stop them before your operation.
Infection
There is a small risk of infection with any operation (about 5-13 cases in 100 operations). If it occurs, an infection can be a wound infection, vaginal infection or a urinary infection, and is usually treated with antibiotics. The risk of infection is reduced by routinely giving you a dose of antibiotic during your operation. Chest infection may also occur because of the anaesthetic.
What can you do?
Treat any infections you are aware of before surgery. After surgery, regular deep breathing exercises can help prevent chest infections; the nurses will guide you how to do this.
Deep Vein Thrombosis (DVT)
This is a clot in the deep veins of the leg. Occasionally this clot can travel to the lungs (pulmonary embolism) which can be very serious and in rare circumstances it can be fatal (<1% in patients who already have DVT). The risk increases with obesity, severe varicose veins, infection, immobility and other medical problems. The risk is significantly reduced by using special stockings and injections to thin the blood.
What can you do?
Stop taking any hormones such as hormone replacement therapy (HRT) and some types of birth- control pills 4 weeks before surgery. These can usually be restarted 4 weeks following surgery when the risk of blood clots has reduced. Do not arrange surgery the day after a long car journey or flight. As soon as you are awake start moving your legs around. Keep mobile once you are at home and continue to wear your compression stockings during times when you are less mobile.
Wound complications
The wound within the vagina can become infected. Occasionally stitches can become loose allowing the wound to open up or on the other hand, tighten up causing discomfort.
What can you do?
Keep the surrounding area clean, and dry carefully after washing using a clean towel or a hairdryer on a cool setting. Do not douche the vagina or use tampons.
General risks of prolapse surgery
Getting another prolapse
There is little published evidence of exactly how often prolapse recurs. Recurrence of the same prolapse probably occurs in about 1 in 10 cases but it is generally believed that about 3 in 10 women who have an operation for prolapse will eventually require treatment for another prolapse. This is because the vaginal tissue is weak. Sometimes even though another prolapse develops it is not bothersome enough to require further treatment.
What can you do?
Keeping your weight normal for your height (normal BMI), avoiding unnecessary heavy lifting, and not straining on the toilet, may help prevent a further prolapse, although even if you are very careful it does not always prevent it.
Failure to cure symptoms
Even if the operation cures your prolapse it may fail to improve your symptoms, eg change in the way your bowel works. Some patients experience worsening constipation following surgery. This may resolve with time. It is important to try to avoid being constipated following surgery to reduce prolapse recurrence.
What can you do?
If you are struggling with constipation after simple changes in diet and fluid intake, your doctor/GP may prescribe some laxatives.
Specific risks of an anterior vaginal wall repair
Damage to bladder
This is a rare complication but requires that the damage is repaired and this can result in a delay in recovery. It is sometimes not detected at the time of surgery and therefore may occasionally require a return to theatre following surgery. A bladder injury will need a catheter to drain the bladder for 7-14 days following surgery but usually there are no long term problems.
Overactive bladder symptoms
Urinary urgency and frequency (with or without incontinence) usually improve after the operation, but occasionally can start or worsen after the operation.
What can you do?
If you experience this, please let your doctor know so that treatment can be arranged.
Stress incontinence
Having a prolapse of the anterior vaginal wall sometimes causes some kinking of the tube through which you pass urine (urethra). This can be enough to stop urine leaks on coughing, laughing or sneezing. By correcting the prolapse this kink gets straightened out and the leaks are no longer stopped. It is difficult to define an exact risk but it is reported to be in the order of 10% (1 in10).
What can you do?
Doing pelvic floor exercises regularly can help to prevent stress incontinence.
Damage to bowel
This is a rare complication but requires that the damaged organ is repaired and this can result in a delay in recovery. It is sometimes not detected at the time of surgery and therefore may occasionally require a return to theatre. If the rectum (back passage) is damaged at the time of surgery, a temporary colostomy (bag) may be required but this is exceptionally rare.
Painful sexual intercourse
The healing usually takes about 6 weeks and after this time it is safe to have intercourse. Some women find sex is uncomfortable at first, but it gets better with time. You will need to be gentle and may wish to use lubrication initially. Occasionally pain on intercourse can be long-term or permanent.
Before the operation – Pre-op assessment:
Usually you are seen in a preoperative clinic some weeks before your planned operation. At that visit you will be seen by a nurse and possibly also a doctor. You will be asked about your general health and any medications you take. Your blood pressure will be checked and you may have tests to assess your heart and breathing. Blood tests will be taken to check you for anaemia and other things according to your medical condition. Swabs may be taken from your nose and groin to make sure that you do not carry MRSA (bacteria that are very resistant to antibiotics and may cause problems after your operation). You may be asked to sign a consent form if this has not been done already.
After the operation – in hospital
Pain relief
An anterior repair is not a particularly painful operation and often includes injection of local anaesthetic into the vaginal tissues during the operation but sometimes you may require tablets or injections for pain relief. Some women describe the pain as similar to a period. It is often best to take the pain killers supplied to you on a regular basis aiming to take a pain killer before the pain becomes a problem.
Drip
You may have a drip after the operation; this is to keep you hydrated until you are drinking normally. The drip is usually removed within 24 hours.
Catheter
You may have a tube (catheter) draining the bladder. The catheter may give you the sensation as though you need to pass urine but this is not the case. It is usually removed the morning after surgery or sometimes later the same day.
Pack
Some gynaecologists insert a length of gauze into the vagina at the end of the operation. It acts as a pressure bandage and is usually removed the following day.
Vaginal bleeding
There may be slight vaginal bleeding like the end of a period after the operation.
Eating and drinking
You should be able to drink and eat within a few hours of returning to the ward.
Preventing DVT (deep vein thrombosis)
You will be encouraged to get out of bed soon after your operation and take short walks around the ward. This improves general wellbeing and reduces the risk of clots in the legs. You may be given a daily injection to keep your blood thin and reduce the risk of blood clots until you go home or for longer in some cases.
Going home
You are not usually in hospital for more than one or two days and may go home the same day. If you require a sick note or certificate please ask.
After the operation – at home
- Moving around is very important; using your leg muscles will reduce the risk of clots in the back of the legs (DVT).
- Bath or shower as normal.
- Do not use tampons for 6 weeks and avoid douching the vagina.
- Any of the stitches under the skin will melt away by themselves. The surface knots of the stitches may appear on your underwear or pads after about two weeks, this is quite normal. There may be a little bleeding again after about two weeks when the surface knots fall off, this is nothing to worry about.
- You are likely to feel tired and may need to rest in the daytime from time to time for a month or more, this will gradually improve.
- It is important to avoid stretching the repair particularly in the first weeks after surgery. Therefore, avoid constipation and heavy lifting. The deep stitches dissolve during the first three months and the body will gradually lay down strong scar tissue over a few months.
- Avoid constipation.
- Drink plenty of water / juice.
- Eat fruit and green vegetables, especially broccoli.
- Plenty of roughage e.g. bran / oats.
- Any constant cough is to be treated promptly. Please see your GP as soon as possible.
- At six weeks gradually build up your level of activity.
- After 3 months, you should be able to return completely to your usual level of activity.
- You should be able to return to a light job after about six weeks, a busy job in 12 weeks. Avoiding unnecessary heavy lifting will possibly reduce the risk of the prolapse recurring.
- You can drive as soon as you can operate the pedals and look over your shoulder without discomfort, generally after three weeks, but you must check this with your insurance company, as some of them insist that you should wait for six weeks.
- The healing usually takes about 6 weeks and after this time it is safe to have intercourse. Some women find sex is uncomfortable at first but it gets better with time. Sometimes the internal knots could cause your partner discomfort until they dissolve away. You will need to be gentle and may wish to use lubrication initially. Occasionally pain on intercourse can be long-term or permanent.
- You usually have a follow up appointment anything between 6 weeks and six months after the operation. This may be at the hospital (doctor or nurse), with your GP or by telephone. Sometimes follow up is not required.
See also information provided by the Royal College of Obstetricians and Gynaecologists: Pelvic floor repair operation – recovering well
What to report to your doctor after surgery
- Heavy vaginal bleeding
- Smelly vaginal discharge
- Severe pain
- High fever
- Pain or discomfort passing urine or blood in the urine
- Difficulty opening your bowels.
- Warm, painful, swollen leg
- Chest pain or difficulty breathing
Treatment Alternatives
Non-surgical
- Do nothing – If the prolapse is not too bothersome then treatment is not necessarily needed. If, however, the prolapse permanently protrudes through the opening to the vagina and is exposed to the air, it may become dried out and eventually ulcerate. Even if it is not causing symptoms in this situation it is probably best to push it back with a ring pessary (see below) or have an operation to repair it. Weight reduction in overweight women and avoiding risk factors such as smoking (leading to chronic cough), heavy weight lifting jobs and constipation may help with symptom control. The prolapse may become worse with time but it can then be treated.
- Pelvic floor exercises (PFE) – The pelvic floor muscles support the pelvic organs. Strong muscles can help to prevent a prolapse dropping further. PFEs are unlikely however, to provide significant improvement for a severe prolapse where the uterus is protruding outside the vagina. A women’s health physiotherapist can explain how to perform these exercises with the correct technique. It is important that you try the pelvic floor exercises to help to manage the symptoms of your prolapse and to prevent it becoming worse. It is also very important to continue with your pelvic floor exercises even if you have opted for other treatment options.
- Pessary – A vaginal device, a pessary may be placed in the vagina to support the vaginal walls and uterus. A pessary is usually used continuously and changed by a doctor or nurse every 4-12 months depending upon the type used and how well it suits you. Alternatively, if you prefer, you may be taught to replace the pessary yourself. It is possible to lead a normal life with continuation of activities such as bathing, cycling, swimming and, in some cases, sexual intercourse. Ongoing care is often at the GP practice but some women will need to be kept under review in the Gynaecology clinic. Pessaries are very safe and many women choose to use one long term rather than have an operation. On occasions their use has to be discontinued due to bleeding, discharge, sexual difficulties or change in bladder function but these all stop quickly after removal. Sometimes it will take several visits to the clinic to determine the best size for you but a pessary is not suitable for all women.
More information
If you would like to know more about uterine prolapse and the treatments available for it you may try the following sources of information.
- Ask your GP
- Ask the Doctor or Nurse at the hospital
- Look at a websites such as:
- The NHS website – NHS (www.nhs.uk)
- Patient UK at http://patient.info/health
- Royal College of Obstetricians and Gynaecologists patient information
- International Urogynaecology Association (IUGA) patient information leaflet
